An Interview with Richard H.Rahe, M.D.
By Paul J. Rosch, MD, F.A.C.P.
This interview was featured in the August 2007 issue of
Health and Stress, the Newsletter of The American Institute of Stress
[divider /]
As the 19th century mathematician physicist Lord Kelvin emphasized, “To Measure Is To Know”, but there are numerous ways to measure “stress”. You can measure hormone levels in body fluids, cardiovascular and electrodermal responses to stimuli, other changes in sympathetic and parasympathetic balance that affect blood flow in the extremities, face or speech, and by using sophisticated EEG and imaging techniques that show specific changes in the brain. The most cost effective and therefore the most commonly used measures are self report questionnaires, many of which have been designed to measure stressful states and traits such as anger, anxiety, depression and Type A coronary behavior. The gold standard in questionnaires to measure stress is generally called the Holmes-Rahe scale, first published 40 years ago, and which has subsequently been revised and updated several times by Dr. Rahe. Before discussing the evolution of this rating scale, it is important to explain some of the difficulties encountered in this undertaking and to provide some historical background.A major problem is that stress is difficult to define in objective terms that scientists can agree on because it differs for each of us. Things like a steep roller coaster ride, bungee jumping or sky diving that would be very distressful for many people are exhilarating and highly pleasurable for others. We also respond differently to stress. Some people blush but others become pale. Hans Selye, who coined the term “stress” as it is currently used, struggled unsuccessfully all his life to find a satisfactory definition. As he frequently complained to me, “Everyone knows what stress is, but nobody really knows.” So, if you can’t define stress, how can you possibly measure it? As Lord Kelvin also noted, “You can’t improve anything if you can’t measure it”. And the same applies if you want to reduce anything, and this is especially true for stress.Although these hurdles make it difficult to prove that stress can cause or contribute to illness, evidence for such a relationship has been recognized and widely accepted in all cultures since antiquity. Over 2000 years ago, Galen not only emphasized the need for equilibrium in the four humors to preserve health, but also what he called the “non-naturals”, among which he included the “passions or perturbations of the soul.” It was equally important to help patients keep their emotions in balance to preserve mental as well as physical health. This belief in the influence of strong emotions on health and illness grew progressively stronger in the Medieval period and was championed by Moses Maimonides, the 12th century physician, philosopher and rabbi, who was the leading medical figure of his day. He was so celebrated, that despite being Jewish, he was physician to Saladin, the Sultan of Egypt, whose huge empire at the time of the Crusades included Syria, Iraq, Mesopotamia, Jordan, Jerusalem and Mecca. Maimonides wrote, “It is known … that passions of the psyche produce changes in the body that are great, evident and manifest to all. On this account … the movements of the psyche … should be kept in balance … and no other regimen should be given precedence.” As a result, “The physician should make every effort that all the sick, and all the healthy, should be most cheerful of soul at all times, and that they should be relieved of the passions of the psyche that cause anxiety.”The importance of emotional balance and mind-body relationships was increasingly recognized during the Renaissance when fears about the influence of the “imagination” were intense. It was widely believed that vivid thoughts and ideas could cause serious problems, especially during pregnancy, where the effects were sometimes bizarre.
Frog Baby
 Ambroise Paré, the famous 16th century surgeon who revolutionized the treatment of wounds, reported several cases in his 1585 Oeuvres(Collected Works). The “frog baby” born in 1517 was thought to be a prime example of the power of a pregnant woman’s imagination. The mother was advised to hold a live frog in her hand to cure her fever and had been holding it when she became pregnant. In addition to the child “having the face of a frog” shown to the left, another baby was born with the body of a calf. His subsequent 1573 book, Des Monstres et Prodiges, contained numerous additional accounts and illustrations of grotesque human-animal forms of life. It is believed to have been the source for Caliban, described as being a “savage and deformed slave” in Shakespeare’s The Tempest, published 50 years later.Robert Burton’s The Anatomy of Melancholy, published in 1621, warned that, “the mind most effectually works upon the body, producing by his passions and perturbations miraculous alterations … cruel diseases and sometimes death itself.” These beliefs in the power of imagination and strong emotions to influence the onset and course of illnesses persisted in medical textbooks, essays and monographs over the next two centuries and were emphasized in Dr. William Falconer’s 1788 A Dissertation on the Influence of the Passions Upon the Disorders of the Body.The discovery that bacteria could cause disease, Koch’s postulates, improved microscopes that facilitated pathological diagnoses, and other 19th century scientific advances shifted the focus away from mental and emotional causes of illness. However, Charcot and his student Freud had become interested in the phenomenon of hysteria and using hypnosis to treat it by identifying and removing repressed memories of traumatic events that appeared to be causing hysteria in some patients. Freud later replaced hypnosis with his “talking cure”, which was later called psychoanalysis. During World War I Freud’s ideas about the emotional origins of hysterical symptoms were often applied to “shell-shock” and other “war neuroses” for which no organic basis could be found, and that now fall under the diagnosis of Post Traumatic Stress Disorder. In 1930, Franz Alexander, a graduate of the Berlin Psychoanalytic Institute and brilliant disciple of Freud, was invited to the University of Chicago, where the first University Chair of Psychoanalysis ever had been established. Two years later, he founded the Chicago Psychoanalytic Institute, which soon achieved international renown as an outstanding psychoanalytic training and research center, and whose graduates included Karl and William Menninger.Alexander made a careful distinction between classical conversion hysteria and what he called “organ neuroses” due to automatic autonomic nervous system mechanisms that controlled emotional and other responses to stressful stimuli. Often called “The Father of Psychosomatic Medicine”, he assembled investigators from various clinical and laboratory disciplines at his Institute. This led to similar research groups that were developed elsewhere, such as the one headed by Stanley Cobb at the Massachusetts General Hospital. In addition, Flanders Dunbar at Columbia Presbyterian Medical Center in New York City, whom I later had the privilege of collaborating with, had produced a masterful monograph, Emotions and Bodily Changes: A Survey of Literature on Psychosomatic Interrelationships. Her subtitle gave this growing movement a name by introducing the term “psychosomatic” into American Medicine. Four years later, in 1939, Psychosomatic Medicine was founded as the first medical journal devoted specifically to publishing research in this rapidly expanding field.
Ambroise Paré, the famous 16th century surgeon who revolutionized the treatment of wounds, reported several cases in his 1585 Oeuvres(Collected Works). The “frog baby” born in 1517 was thought to be a prime example of the power of a pregnant woman’s imagination. The mother was advised to hold a live frog in her hand to cure her fever and had been holding it when she became pregnant. In addition to the child “having the face of a frog” shown to the left, another baby was born with the body of a calf. His subsequent 1573 book, Des Monstres et Prodiges, contained numerous additional accounts and illustrations of grotesque human-animal forms of life. It is believed to have been the source for Caliban, described as being a “savage and deformed slave” in Shakespeare’s The Tempest, published 50 years later.Robert Burton’s The Anatomy of Melancholy, published in 1621, warned that, “the mind most effectually works upon the body, producing by his passions and perturbations miraculous alterations … cruel diseases and sometimes death itself.” These beliefs in the power of imagination and strong emotions to influence the onset and course of illnesses persisted in medical textbooks, essays and monographs over the next two centuries and were emphasized in Dr. William Falconer’s 1788 A Dissertation on the Influence of the Passions Upon the Disorders of the Body.The discovery that bacteria could cause disease, Koch’s postulates, improved microscopes that facilitated pathological diagnoses, and other 19th century scientific advances shifted the focus away from mental and emotional causes of illness. However, Charcot and his student Freud had become interested in the phenomenon of hysteria and using hypnosis to treat it by identifying and removing repressed memories of traumatic events that appeared to be causing hysteria in some patients. Freud later replaced hypnosis with his “talking cure”, which was later called psychoanalysis. During World War I Freud’s ideas about the emotional origins of hysterical symptoms were often applied to “shell-shock” and other “war neuroses” for which no organic basis could be found, and that now fall under the diagnosis of Post Traumatic Stress Disorder. In 1930, Franz Alexander, a graduate of the Berlin Psychoanalytic Institute and brilliant disciple of Freud, was invited to the University of Chicago, where the first University Chair of Psychoanalysis ever had been established. Two years later, he founded the Chicago Psychoanalytic Institute, which soon achieved international renown as an outstanding psychoanalytic training and research center, and whose graduates included Karl and William Menninger.Alexander made a careful distinction between classical conversion hysteria and what he called “organ neuroses” due to automatic autonomic nervous system mechanisms that controlled emotional and other responses to stressful stimuli. Often called “The Father of Psychosomatic Medicine”, he assembled investigators from various clinical and laboratory disciplines at his Institute. This led to similar research groups that were developed elsewhere, such as the one headed by Stanley Cobb at the Massachusetts General Hospital. In addition, Flanders Dunbar at Columbia Presbyterian Medical Center in New York City, whom I later had the privilege of collaborating with, had produced a masterful monograph, Emotions and Bodily Changes: A Survey of Literature on Psychosomatic Interrelationships. Her subtitle gave this growing movement a name by introducing the term “psychosomatic” into American Medicine. Four years later, in 1939, Psychosomatic Medicine was founded as the first medical journal devoted specifically to publishing research in this rapidly expanding field.
World War II accelerated the growth of psychosomatic medicine even further as psychiatrists and others trained in this discipline were mobilized to treat shell shock and similar symptoms. Grinker and Spiegel’s 1945 Men Under Stressdetailed these experiences and in 1943, Weiss and English’s Psychosomatic Medicine and Dunbar’s had also attracted a large medical audience. Scientific studies skyrocketed and medical schools created new programs for their curriculum to satisfy the demand for more information on mind/body relationships. Psychosomatic medicine was so much the “rage” at mid-century, that popular magazines constantly ran relevant articles and psychosomatic theories were featured in the lyrics of Guys and Dolls (“In other words, just from waiting around for that plain little band of gold, A person can develop a cold.” Adelaide’s Lament). The play won five Tony Awards, ran on Broadway for well over three years, and was later made into an award winning movie that included Marlon Brando, Frank Sinatra and other stars. By the time the Holmes-Rahe life events scale was published in 1967, there was also a huge lay audience thirsty for such information and it also received enormous media coverage, including Timemagazine, the popular syndicated Dear Abby column and Alvin Toffler’s Future Shock. In that regard, Stewart Wolf, who was well acquainted with its origins as well as Tom Holmes and Richard Rahe, once told me that it should have been called the Rahe-Holmes scale. I suspect that after the following interview with Richard Rahe, you will understand why.
PJR: I suspect that most people are familiar with your name because of the (SRE) Schedule of Recent Events approach and the Holmes-Rahe rating scale (SRRS) Social Readjustment Rating Scale that has been a gold standard of stress assessment for four decades. As a result, they may be unaware of your many other achievements. I first met Tom Holmes in 1951, when I had a Fellowship with Hans Selye, and we visited him at New York Hospital during his return visit from The University of Washington. He had been a member of the “Wolffpack”, a group of physicians under the tutelage of Harold Wolff at Cornell that included other pioneers in psychosomatic medicine like Stewart Wolf, George Wolf and Larry Hinkle. Tom was interested in the relationship between allergic rhinitis and stress, which was allegedly kindled by the observation that he usually developed a cold when his mother-in-law came to stay with him for a week or more. The clear relationship between the frequency and severity of colds and the magnitude of stress has since been confirmed in numerous studies. His book, The Nose, had recently been published, showing that nasal responses to stimuli or stress almost always involved changes in deeper respiratory function and often affected other organs and systems. Like Stewart Wolf, Tom became a good friend as well as a very early Member of the Board of Trustees of The American Institute of Stress. I think it would be of interest to our readers to learn how you became associated with him and how the Holmes-Rahe Scale was born.
RHR: Thanks Paul. I might first point out the differences between the SRRS and the SRE. The SRRS presents average magnitudes for 42 life change events and is often called the Holmes-Rahe scale. The SRE was the initial research instrument used at the University of Washington to collect subjects‘ recent life changes information.Here’s the story of how the SRRS came into being. At the University of Washington School of Medicine, first and second year students could apply for a small research grant to work within a department of their choice during summer vacation. My first summer I worked with Robert Rushmer, a noted cardiovascular researcher. The second summer was spent in psychiatry with Thomas Holmes. He first suggested that I review all the life changes and illness papers coming from the Department of Psychiatry. I did so and wrote a review article, where, among other issues, I pointed out that in many of these articles, recent life changes were measured differently. Most often, simple counts of the number of changes were used, but none of the methods differentiated between severe life changes, like death of a spouse, from minor changes, such as a vacation.On my Psychiatry rotation as a third year student, Dr. Holmes and I had attended a presentation by Eugene Galanter, PhD, on scaling the severities of juvenile crimes using a proportionate scaling technique devised by his mentor, E.E. Stevens. On the way back from the talk, Dr. Holmes speculated that this scaling method might be an answer to my review article critique. All Tom needed to do was to suggest this possibility and I quickly volunteered to conduct such a scaling study. It took me two years to collect all the data from over 400 subjects of differing ages, gender, education, race, and social status. I did the first analyses of these data by sorting questionnaires into various demographic groups on the living room floor of my apartment. Later on, I obtained funding for a computer scientist to collate all this information. I finally submitted the report in a publishable form at the end of my fourth year of medical school. Although Tom assiduously edited my drafts, he always left the work to me. As Professors mentoring young investigators often did in those days, Tom said to me, “For your first two papers you were the first author. I think I’ll put my name first on this one.” I later discovered he had done the same with a sociologist graduate student who studied life changes in patients prior to the onset of tuberculosis. This common academic practice ultimately led many peer reviewed journal editors to begin requiring authors to specify their individual contributions to a submitted manuscript.
After graduation I did a straight medicine internship on Cornell University’s wards at Bellevue Hospital in New York City. I had intended to become a medical resident under Harold Wolff, but he died the day before I was to first meet him to present a case of hyperthyroidism seemingly brought on by severe recent life stresses. I changed my residency to Psychiatry and returned to the University of Washington. During my residency I continued to conduct studies of recent life changes and illness onset for colleagues who were willing to help me. I developed the Life Change Unit (LCU) concept to measure the magnitude of life changes and in prospective studies, the higher the residents’ LCU score reported for the year prior to study, the greater were the numbers of reported illnesses over the following year. Residents with life changes totals from 0 to 150 were generally healthy the following year and those with totals from 151 to 300 tended to report one or two minor illnesses. However LCU’s greater than 300 over the previous year were frequently associated with multiple minor illnesses and occasionally a severe illness over the following 12 months. Tom held on to these two papers saying that he wanted to replicate them before publishing. After two more years and no action on his part, I published the material as a chapter in a book.
PJR: You were able to continue your research while on active duty in the Navy and modified the SRE to make it more meaningful for naval personnel. You rescaled your original 42 life change events along with 12 new military related events in 1980. In 1997 you had added a total of 36 new life changes to the original 42 and did another rescaling experiment with a group of subjects carefully selected to closely match the original sample in number, age, education, race, religion, and socioeconomic status. That same year, you presented and discussed the results of these changes at our Ninth International Congress on Stress in Switzerland. Of particular interest was the observation thatLCU values for the original 42 events listed in 1967 had increased on average by 45 percent over the next thirty years! I emphasize this since I see so many articles in lay and even medical publications that still use the original Holmes-Rahe scale to assess stress, or cite it as the preferred measure, and are unaware of important updates you have periodically made over the past four decades.
With respect to your early work in the Navy I also recall that you did some studies with patients recovering from a heart attack that later led to further stress and coronary heart disease investigations in Sweden. This work resulted in contacts with Ray Rosenman, Stewart Wolf, Töres Theorell, Lennart Levi and other mutual friends, who, like yourself, have contributed so much to our International Congresses on Stress. How did this set of fortunate circumstance come about?
RHR: My research at the University of Washington had attracted the interest of Ransom J. Arthur, M.D., Commanding Officer of the Navy Medical Neuropsychiatric Research Unit in San Diego, California. I was due to spend two years on active duty following my residency and Dr Arthur arranged for me to be assigned to this facility. Here I was able to conduct a variety of life changes and illness studies utilizing several Navy populations, including Underwater Demolition Team (UDT) Trainees, Naval Aviators, Navy Submariners, and Naval Officers and enlisted men aboard two heavy cruisers and an aircraft carrier. It proved necessary to alter the SRE for better application to these military populations. Recent life changes magnitudes were summed over 2 years, 1 year, and 6-month intervals to see which time interval was most predictive of near-future illness. Dr. Arthur and I decided to label these values life change units, or LCU. In one major study I followed over 1,000 Naval officers and enlisted men on a 6-month shipboard cruise. Each man’s LCU total for the year prior to the cruise was obtained along with all illnesses that each man experienced throughout the cruise. As illnesses of any significance were routinely reported to sick-bay aboard ship for treatment, illness data could be collected in this study without having to rely on subjects’ memories. These shipboard results proved to be extremely similar to those that I found in my studies of medical residents mentioned above. It was of great interest to me to see these early life change and subsequent illness studies supported in Sheldon Cohen’s recent paper three decades later. Cohen examined volunteers’ antecedent life change intensities and found them significantly related to their subsequent development and severity of an induced upper respiratory infection.
When I completed my obligatory two years of active duty in mid 1967, I extended my tour for another year to continue my studies of patients recovering from a heart attack at the San Diego Naval Hospital. I had uncovered evidence of elevated recent life change magnitudes in patients’ lives over the year preceding their infarctions. I received advice and encouragement from Meyer Friedman, Ray Rosenman, Larry Hinkle and Stewart Wolf at meetings of the American Psychosomatic Society to pursue this research. Stewart proposed that I apply for an NIMH Special Fellowship to study life changes and coronary heart disease at the Karolinska Institute in Stockholm, Sweden under Gunnar Biorck, M.D. Gunnar was Chief of Cardiology at the Serafimer hospital, where all cardiac patients in the city of Stockholm were referred for treatment. I received the NIMH award in 1968 and spent the next 15 months conducting several life changes and coronary heart disease studies with four of Gunnar’s MD/PhD candidates. One of these candidates was Töres Theorell. I also met Lennart Levi, who was then completing his PhD work and he referred to some of my published papers in his thesis.
PJR: Please tell us a little more about your studies in Sweden and particularly your association with Töres Theorell, who followed Lennart as Director of this important and very productive Division of Psychosocial Factors and Health at Karolinska. At our 1997 International Congress on Stress, when you were the recipient of our Hans Selye Award, several co-workers paid homage to your achievements. I was particularly impressed with Töres’ presentation on “Life Stress And Coronary Heart Disease In Sweden” as being a generous and appropriate tribute. I recall that you coauthored several papers with him and also collaborated with Ray Rosenman and others on various aspects of stress and heart disease that would be of interest to our readers.
RHR: Over my 15 months in Stockholm (1968-1969), I designed both retrospective and prospective studies of life change experiences both preceding and following a myocardial infarction with Johannes Paasikivi, Töres Theorell, and Ingvar Liljefors. I also carried out investigations of the build-up of life change events prior to sudden cardiac death with Evy Lind. I met with other Scandinavian scientists during this time and to my delight, many of my Swedish results were later replicated by researchers in Finland and Norway. My collaboration with Töres Theorell continued over many years after my return to active duty at the Navy Research Unit in 1969. Töres made visits to the USA to spend time at my laboratory and later to carry out a lengthy data review with Stewart Wolf. I eventually decided to complete 20 years of active Navy duty, retiring in 1986. I was allowed to continue at the Research Unit until completion of my three years as Commanding Officer in 1980. I was then a Captain and was sent to run Navy Hospitals from 1980 to 1984. My final two years were spent as a Professor at the Uniformed University for the Health Sciences in Bethesda, Maryland where I started a Military Stress Studies Unit that remains very active to this day.
Back in 1969, I had reestablished connections with Ray Rosenman and Stewart Wolf. Ray and I published a paper on the heritability of Type A behavior, as I had previously done work in Sweden on this topic. Around this time, I also started a five-year, randomized, controlled trial of psycho-educational therapy for post myocardial infarction patients beginning shortly after their discharge from the hospital. Five, one-hour, group sessions were devised to introduce them to stress assessments and stress reduction techniques. Meyer Friedman was beginning his long-term study of psychological intervention for Type A Behavior patients following an infarction and encouraged my efforts. The outcome of my study was that patients in my treatment group developed significantly fewer re-infarctions and showed a significantly lower mortality rate compared to controls over a four to five year follow-up interval. One great advantage of studying Naval personnel was the ability to obtain near-complete follow-up data – as most all of my patients continued receiving their cardiac care at the San Diego Naval Hospital.
PJR: My recollection is that you also measured serum cholesterol and uric acid levels in heart attack patients. What was the reasoning behind this and did you learn anything? Later on, you started to study prisoners of war returning from the Vietnam conflict as well as military and civilian hostages held captive in Iran. You also developed group treatment programs for these and others suffering from what is now called PTSD or Post Traumatic Stress Disorder. PTSD has been skyrocketing because of the war in Iraq and an increase in terrorist and violent acts such as 9/11, the Columbine massacre, as well as catastrophic natural disasters like Katrina. The problem is further complicated by confusion with respect to diagnosis and lack of access to adequate treatment. What has your experience been in these areas?
RHR: Ransom Arthur wished to create a “Biochemical Correlates Laboratory” at the Research Unit. Ransom and I had carried out studies of serum uric acid and serum cholesterol with Navy frogmen over their four months of UDT (Underwater Demolition Team) training in 1966 and 1967. In 1968 Robert Rubin, MD, PhD came to the Research Unit for his two years of active duty. Bob had previously studied stress and serum cortisol at UCLA and it seemed desirable to include cortisol analyses in our UDT database. Ransom appointed me as Head of this Biochemical Correlates Laboratory and, whenever possible, I measured serum uric acid, cholesterol, cortisol, and later salivary testosterone levels in my stress studies. What became clear from several investigations was that serum uric acid levels generally peaked for subjects immediately prior to their taking on a very stressful challenge. In most instances, the higher the peak the better was their performance. In later work, we surmised that these uric acid increases were likely the result of decreased serum volume of the body due to an elevation in catecholamines resulting in vasoconstriction. From our total cholesterol data we found marked elevations for subjects showing difficulties coping with current life stresses. Cholesterol concentrations were particularly high for subjects who were actually failing in their coping efforts. This was in the days before high and low density lipoprotein measurements were readily available. In terms of serum cortisol results, rather than finding short-term rises for persons at the beginning of a life challenge, as had been reported by others, we discovered levels which were twice the upper limit of normal that persisted over four weeks of demanding UDT training. Bob Rubin still continues investigations of subjects’ estrogen and testosterone variability under stress.
In the early 1970s, Ransom Arthur began preparations for a comprehensive medical program that would both evaluate and, when necessary, provide treatment for returned prisoners of war from Vietnam. Army, Navy, and Marine POWs were to be seen at the Naval Hospital in San Diego and Air Force POWs would be transported to Brooke Army Medical Center in San Antonio. I helped design the psychiatric evaluation portion of this program and when the POWs were returned in 1973, I was among the psychiatrists selected to be an interviewer. In addition, when Iranian political activists occupied the American Embassy in 1980, I was one of the Department of Defense/Department of State psychiatrists assigned to debrief the 52 former captives over a five-day evaluation at the Air Force Hospital in Weisbaden, Germany. I learned a great deal about both successful and unsuccessful coping with severe stress from these former captives. I learned a great deal about both successful and unsuccessful coping with this type of severe stress from former captives. Using this information, I modified my 5 psycho-educational sessions for post myocardial infarction patients and adapted it for use with these and other severe trauma survivors. I developed my Stress and Coping Inventory (SCI) to assist in this treatment, and for some individuals, I also used a modified version of Adolf Meyer’s Life Chart to portray their life stresses, coping, and illness experiences.
PJR: I know that you continued your research in this area and added further measurement refinements and in recent years have focused on improving the understanding of PTSD and therapy techniques. However, I don’t want to jump ahead too fast and we will return to this later. Since many readers may not be familiar with Adolf Meyer’s Life Chart, it might be helpful to explain that Meyer was appointed Chief Psychiatrist at Johns Hopkins Hospital in 1908 and designed its Phipps Psychiatric Clinic in 1913 to integrate teaching, research, and patient care from a psychobiologic approach. Meyer developed the “life chart” approach to depict both biographical and medical information to enable clinicians to appreciate the temporal relationships between patients’ stressors and subsequent illnesses. In his life chart, each year was identified by a new horizontal line and a column on the left listed a patient’s complaints and illnesses and to the right, any psychosocial or environmental changes and their reactions. In between these two columns, curves outlined the growth and maturation of various organs and systems, resulting in a diagram shaped like a torpedo. Harold Wolff taught this “Meyerian torpedo” approach to his group at Cornell, which included Tom Holmes. When Tom went to the University of Washington in 1949, he was assigned to a tuberculosis hospital, and in the early fifties, co-opted Norman Hawkins, who was obtaining his doctorate in sociology to do a study that showed higher rates of infection in patients with low economic status. There was nothing very new about this but Hawkins wondered why others with the same profile did not develop the disease. He postulated that susceptibility was increased by psychosocial stress and his subsequent study confirmed increased clusters of such personal stresses in the years preceding admission. This was reminiscent of Meyer’s life chart findings and in attempting to evaluate stress he concentrated on seven issues that Wolff had emphasized. Hawkins developed a measurement instrument he called the Schedule of Recent Experience (SRE). Hawkins and Holmes then did a prospective study of hospital employees who developed tuberculosis that also found increased SRE measurements in the preceding years. In 1959, Holmes had Thomas Hart, a medical student, do his thesis on another prospective tuberculosis study that used the SRE in addition to other instruments, during which Hart assigned point values to various items. Hawkin’s original SRE and possibly Hart’s modifications were forerunners the Holmes-Rahe Social Readjustment Rating Scale that assigned life change and readjustment points to 42 representative life events. Except for your review article as a medical student, Hawkins and Hart are rarely referred to. My recollection is that your own medical student thesis in 1961 on stress and hernia also followed Meyer’s approach using the SRE. It would be of interest to learn more about these early contributions as well as your magnificent study of Vincent Van Gogh and his life chart.
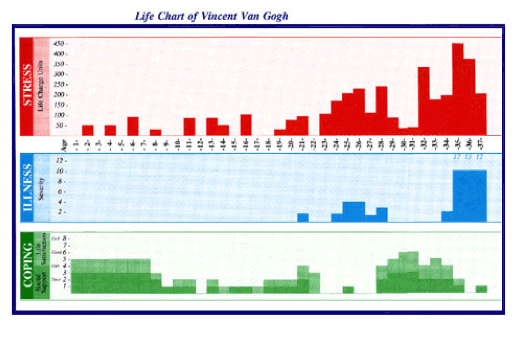
RHR: Tom had all third year medical students on their Psychiatry rotation use the SRE and the Life Chart approach with a patient of their choice. This work-up took about 4 hours of interviewing and another hour to write the report. Tom had simplified the Life Chart to some degree–eliminating the torpedo shaped weights for the body’s organ systems. Students in my class had not been exposed to the Holmes-Rahe SRRS – as I was still in the early phases of that research. It wasn’t until I was taking extensive personal, social, and medical histories of former political captives that I returned to using the life chart. I simplified it further, adding yearly LCU values to the life events column, illness severity units for reported illnesses, and a column for yearly assessments of two aspects of coping – social support and life satisfaction. To illustrate the potential clinical usefulness of these revisions, I constructed a Life Chart for Vincent van Gogh shown below. As you will see, my life chart is horizontal rather than Meyer’s vertical display.
 Stress differs from these and other predisposing factors in that it helps to explain the timing of illness onset and often its severity. Thus, in one respect, stress may be thought of as pulling the trigger of a loaded gun. Episodes of major depression recurred several times in van Gogh’s Life Chart, but the timing of his suicide was clearly linked to the extraordinary increase in life change events, their associated health problems and the almost complete lack of coping skills toward the end of his life. The self-portrait on the left was painted after he had cut off a large portion of his left ear in 1888. It appears to be the right ear because he was probably looking in a mirror at the time he was painting this.
Stress differs from these and other predisposing factors in that it helps to explain the timing of illness onset and often its severity. Thus, in one respect, stress may be thought of as pulling the trigger of a loaded gun. Episodes of major depression recurred several times in van Gogh’s Life Chart, but the timing of his suicide was clearly linked to the extraordinary increase in life change events, their associated health problems and the almost complete lack of coping skills toward the end of his life. The self-portrait on the left was painted after he had cut off a large portion of his left ear in 1888. It appears to be the right ear because he was probably looking in a mirror at the time he was painting this.recipient of the annual Paul J. Rosch Award
As you well know, Ana Maria is a human dynamo and Jim Quick and I marveled at her boundless energy and how she has steadily improved this event so that it has now become an important international event. This year’s event attracted 700 people from Brazil and four other countries including two psychologists from Angola. Redford Williams from Duke, and President of the International Society of Behavioral Medicine discussed “Psychosocial Risk Factors for Cardiovascular Disease” and Ronald Schouten, Director of the Law& Psychiatry Service of the Massachusetts General Hospital and Professor of Psychiatry at Harvard Medical School gave an equally informative presentation on “Assessing and Managing Disruptive Behavior by Executives and Professionals.” Ana Maria is also very excited about your next Congress and is eager to assist in promoting this in any way she can.
PJR: Many thanks. I neglected to mention that in addition to our Hans Selye Award, you have been the recipient of numerous honors, including the Career Achievement Award from the International Critical Incident Stress Foundation, Navy Commendation and Meritorious Service Medals, and have served as President of The Psychosomatic Society and the USA branch of The International Stress Management Association. I am looking forward to your participation in our 12th International Congress on Stress in 2008, where you will have a chance to reunite with old friends and colleagues who are also enthusiastic about participating in and helping to plan this conference, like Herb Benson, Cary Cooper, Lennart Levi, Ken Pelletier, Jim Quick, Ray Rosenman, Charlie Spielberger, Töres Theorell, as well as others I have not yet invited to serve on our Scientific Advisory Board. This will be held for the first time in North America and although the dates and location of this two or three day Congress have not been finalized, the new Wynn hotel in Las Vegas and similar elegant sites in New York or Chicago are among the current leading current contenders. Unlike prior Congresses at Five Star hotels in Switzerland and Hawaii, where space constraints limited attendance and precluded having exhibits, next year’s venue will permit 500 or more registrants and up to 50 exhibits. In addition, it will have an emphasis on Job Stress that will be targeted to a lay audience as well as our usual assemblage of physicians, other health care professionals and researchers. Stay tuned for more information on this exciting event in future Newsletters as well as periodic updates on our web site.