Sensorimotor Psychotherapy: An Alternative for Veterans
*This is an article from the Spring 2021 issue of Combat Stress
By Chris Zaglifa, MSW, LCSW, SAC
As a dual diagnosis clinical social worker primarily trained in Cognitive Behavioral Therapy (CBT) and exposure therapy, it became evident that a percentage of Veterans chose not to engage in these therapies, were unable to tolerate the therapy, or chose to drop out.1 Also evident was a pattern among these Veterans of having multiple co-morbid diagnoses of addiction, insomnia, depression, suicidal behaviors, attention deficit disorder, and a pattern of high Adverse Childhood Experience (ACE) scores.2 Even after completing both residential and outpatient programs, some Veterans, while habituating to a specific trauma, still struggled with very similar complaints: “I just snap and put my fist through a wall; I verbally go off on my wife and children and then try to grab the words back before they hit their target; When it happens, I am beyond exploring the interaction between my thoughts, emotions and behaviors, or using a Cognitive Behavioral Worksheet; I do not go out, have people over, do fun things with my kids; I think about suicide a lot.” These Veterans’ reports were frequent, and more the rule than the exception.
The purpose of this paper is to share the journey over the past five years to find what we therapists were missing; a model that could be incorporated into treatment to better prepare Veterans to engage in cognitive therapies that would be less overwhelming, and that would help to recognize, understand, and intervene in both physical and emotional dysregulation. My goal is to address the co-morbidities, the pattern of suffering from developmental trauma, and the poor attachment experiences these Veterans had as children; the time when self-regulation is developed.3, 4 The model would need to be easily articulated to explain how the brain and body protect themselves. It must also be non-pathological, non-judgmental, and acceptance of a person wherever that person is, in whatever state they present, while ensuring safety, and demonstrating awareness and sensitivity to the military culture.
Sensorimotor Psychotherapy
My search led to familiarizing myself with somatic-oriented therapies that included Somatic Experiencing (SE) and Sensorimotor Psychotherapy (SP).5, 6, 7, 8 It appeared that SP met the desired criteria. Moreover, the Polyvagal Theory was found to be part of SP.9 The concept of the role the body plays in psychological health is not new but was lost when Western philosophy made cognition supreme in understanding human behavior. Leonardo Da Vinci revolutionized art by exploring “…how psychological emotions led to physical motions.”10 He wanted to display emotions in his art and did so through capturing motion in his paintings. Pierre Janet, a French psychiatrist, when writing on traumatized people in 1919 stated, “Such patients as the one who was perpetually trying to guard herself from being struck… are continuing the action, or rather the attempt at action, which began when the thing happened. They exhaust themselves in these everlasting recommencements.”11
The question was how to lower psychological and physiological reactivity and also provide a structure and interventions to help better understand the effects that developmental issues can have upon one’s ability to tolerate extreme stressors such as those traumatic events typically experienced in the military, such as combat responses to catastrophic devastation with major loss of life through war, earthquake, and the many recent hurricanes. Some Veterans who served both in the Middle East and in Haiti found Haiti to be even more traumatic. This article will describe SP and concentrate on its principles, philosophy, orientation, and focus. How Veterans and this therapist experienced the use of SP will be discussed and the feedback Veterans in individual and group treatment shared during the termination phase will be provided.
SP is…”A body-oriented talking psychotherapy that specifically addresses trauma and attachment wounds, emphasizing the body as an avenue for exploration and vehicle for change.”12 Although SP also uses cognitive and psychodynamic-based treatments, it is a more bottom-up rather than top-down approach that also is neuro-biologically informed, incorporating mindful awareness of the present moment. SP can be used in conjunction with other therapies or as a stand-alone treatment. SP expands upon exploration of thoughts and emotions to include physical sensations, five-sense perceptions, and movements. These are referred to as the core organizers. Porges refers to this gut instinct as “neuroception” which is “… the process through which the nervous system evaluates risk, without requiring awareness.”13 It distinguishes what is safe from what is not safe; that is, unresolved traumatic events during which a person was not able to act or to defend oneself or engage in a fight or flight response. When reminded or triggered by an element of the original trauma, such as an image, sound, smell, taste, or tactile contact, the thinking part of the brain may be unable to function, reverting to animal defenses of either a sympathetic nervous system (fight or flight) or parasympathetic response (shut down or play dead.) “One’s thinking or behavior can become disrupted if arousal moves beyond the boundaries of the ‘window of tolerance.’” 14 A person can respond to a situation over and over again when no actual danger is present. The trauma becomes a procedural or implicit memory, sometimes referred to as a muscle memory, which is physically and emotionally expressed and acted upon bypassing a thought or cognitive process. “Thus, when memories of the traumatic experience are activated by an internal cue (e.g., a feeling state) or an external cue (e.g., a look on someone’s face or a certain sound), the survivor feels as though the traumatic experience is occurring in the present moment and utilizes the same defensive reactions that were used at the time of the original event, such as freezing or fighting.”15
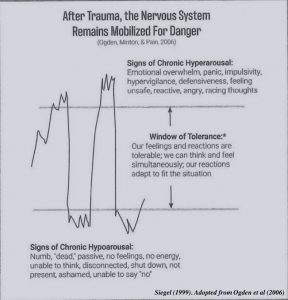
The “Window of Tolerance” (WOT) is an exceptional tool for psychoeducation regarding normal, animal defenses. “In order to put the past in the past, clients must process traumatic experiences in an ‘optimal zone.’”16 Falling between the two extremes of hyper- and hypo-arousal, this zone is described as the WOT. Porges describes this zone as a parasympathetic state called the ventral vagal or social engagement system, where a person can think and feel at the same time. It is bidirectional and can read whether or not another person is safe and able to communicate safety through facial expression and voice. Again, these are normal defense responses that protect the individual. When experiencing a reminder of a traumatic event that was not processed or when trying to put the trauma into words, when the thinking brain is not “online,” these defensive responses can be activated. The thinking brain is not available, and the person remains “stuck” in a perpetual and patterned response as described by Janet.11
The advantage of providing psychoeducation in this manner is non-pathological, non-judgmental, and makes sense out of reactions to stimuli that fall well under the actual presence of a threat. At this point, using a cognitive approach might be counter-productive for those who become easily overwhelmed and again, are unable to put the experience into words. This is not avoidance. “Once these triggers and signs of even slight dysregulation are identified, these clients will benefit from the neural exercises that bring arousal into the window of tolerance and thus, enable prosocial behavior. No matter if triggers are trauma or attachment-related or both, understanding the automaticity of faulty neuroception challenges cognitive schemas of defectiveness, inadequacy and unworthiness.”17
There is a structure to SP, but there is no “typical session,” as the therapy is not manualized nor directed by the therapist. The therapist is not there to direct the therapy, but rather to facilitate clients finding what needs to be accomplished from within themselves. Interventions and resourcing are considered “experiments” and there is no right or wrong, but a curious and mindful approach that will assist as an individual develops a sense of what issues needs to be addressed.
The client is always reminded that if something does not feel right, to stop. The session is then structured for the client to remain in the present. Signs and symptoms of dysregulated behavior are tracked and contacted by being present, connected, attuned and resonating in a non-judgmental manner through contact statements, not questions, that bring a person’s attention to present moment experience. Non-verbal communication, tone of voice and body language that reflect a felt sense of understanding, resulting in engaging the social engagement system. A piece or a sliver of what arises is framed and through mindful questions and directions, brought into awareness and studied, slowly at a tolerable level. The individual can then process them and while being mindfully aware of them, begin to transform these reactions, to think and feel while working the edges of the WOT. The therapist will assist by preventing the patient from completely leaving the WOT. Resources are implemented to assist the patient from becoming hyper- or hypo-aroused. An example would involve changing a person’s posture from being slumped, leaning forward, with feet tucked under the chair, to sitting upright, elongating the spine, and feeling the back of the chair seat. The client can be asked to feel the floor with one’s feet to become grounded and to place one hand on the abdomen and the other on the chest to feel more centered. The client is asked to notice any changes in their breathing, heart rate, muscle tension, etc. When there is a truncated, unexpressed action that occurred during the trauma, the client is given the opportunity to complete that action. For example, the patient or client may do so by reaching out or pushing back or away from an object being held by the therapist, while applying just the right amount of resistance requested by the client to complete the action that was not possible at the time of the trauma. This is called the “Act of Triumph.”18 These are examples of the “experiments” that can be used to allow for the integration of the experience and the transformations achieved brought into one’s daily life.


There are three phases of treatment that are implemented throughout the body.19 In Phase I, the person is kept within their WOT as they become aware of their body and identify any hyper- or hypo-arousal. In Phase 2, the unintegrated memory fragments and core organizers are processed. “Through awareness of the physical impulses that emerge when the memory is evoked, clients find and complete the innate ‘acts of triumph,’ the mobilizing defenses that were ineffective at the time of the original trauma.”20 In Phase 3, resources are used to develop the skills needed to keep the activation of the sympathetic nervous system, mobilization (fight or flight) and parasympathetic immobilization (submit or shut down) within the WOT. Once the client has arrived at this point, cognitive approaches can be implemented as the he or she is able to think and feel at the same time.
Summary of the Foundation and Six Principles of SP.21
The most profound effect the Veterans I treated and upon me were the Foundations and the Six Principles of SP. The Foundations and Principles provided both the philosophical and spiritual ground for clinical practice, laid out the orientation for the therapist, and demonstrated a paradigm for healing, a way of being in relationships, of being with ourselves and others, and seeing the body as a resource.
The Foundations explore the organization of experience, and the need for an Experimental Attitude in lieu of talking or conversing.
- Unity recognizes how we are interrelated and is experienced through communication. It recognizes individual and group differences. A central goal is to facilitate communication between parts of the whole. It is a non-hierarchical approach.
- Organicity refers to the inherent intelligence within every living system to evolve. The power to heal resides in the person, not the therapist. The therapist is alert to this natural process and helps a person explore within themselves and to find their own path. The clients are to change for themselves. Culture and social location are also recognized.
- Mind/Body/Spirit Holism recognizes that in all significant bodily experiences, in addition to a cultural component, there are mental, emotional and spiritual components. SP values the body as a source of primary intelligence, information, and change. The main perspective is the whole person.
- Non-violence refers to the assumption of a non-judgmental attitude. The therapist is the compassionate person and refrains from efforts to manage, direct, or change a person’s behavior or experience.
- Mindfulness/Presence encompasses dual awareness of being both observer and observed without judgment. It pays attention to “what is.” Presence is seen as being with the client, engaged, responsive to the moment, and open in a unified state. It is conducive to intuition and inspiration instead of logic and analysis. This also applies to the therapist, as he or she becomes aware of how the session affects the therapist, while never losing focus on the client.
- Relational Alchemy emerges from the relationship and how the implicit selves interact. This can be challenging, as well as positive. Enactments are viewed as a time when both therapist and client process an interaction, which leads to a higher degree of organization and growth for both parties.
At first, these principles were not well understood, as they were perceived at a cognitive level. However, as I adopted them in practice, I noticed changes within myself at many different levels, as well as change in the Veterans with whom I worked. They began to feel safer and became more open, able to stay in the moment—their WOT—and thus, were able to process more of their trauma-related reactions. The psychoeducation portion brought about a normal defensive response to trauma, a greater self-acceptance, and comfort within themselves. One Veteran, having a bad day and using the language of the WOT, reported, “I lost my WOT. Someone accidentally covered it with a pencil so I could not see it.”
During the termination process, the Veterans offered feedback about their treatment, describing these same principles as they unfolded during the course of treatment. Unity was seen in the groups as they could act as one and accept and honor their differences. They shared the commonly held belief that they knew best what was needed, the therapist helping them to find that innate wisdom of the body. The non-violence was seen as the absence of therapist-directed treatment. Most, if not all, made reference to the fact that they were not judged, were accepted, and were never told what to do or that they “have a problem.” In terms of mind, body, and spirit holism, they commented about being acknowledged as a whole person.
Summary
The question is not which treatment model works the best, but which treatment models, working in unison with the wisdom of other treatment models, will work with each individual. The more inclusive the treatment model, the more success will be realized.
Moreover, the whole person must be taken into consideration. This includes not only the mind, but body, spirit, culture, and lifelong experiences that shape an individual. It also includes an awareness of how each person organizes the self around these experiences to defend oneself and to develop a more balanced and nuanced world view, and the ability to better distinguish present experience from past traumas and threats. Sensorimotor Psychotherapy, along with other somatic-based, body-oriented psychotherapies, adds the component of working with and through the body. Additionally, it facilitates working with slices of the traumatic experience to both complete unresolved and unprocessed actions during a traumatic event through an Act of Triumph and to help the individual find the missing attachment experiences. The Principles of SP can guide treatment providers to safely and successfully work with traumatized patients, allowing them to become aware of their physical reactions and attachment wounds, integrate both body and mind, and reach a transformation that can be practiced and lived in daily life.
REFERENCES
- Gaston, L. Adverse effects of trauma-focused therapies (Part 1). Combat Stress, 2020, Summer.
- Cabrera, O.A., Hoge, C.W., Bliese, P. D., Castro, C.A., and Messer, S. C. Childhood adversity and combat as predictors of depression and post-traumatic stress in deployed troops. American Journal of Preventive Medicine. 2007, 33 (2): 77-82.
- Butterfield, M.I., Lapp, K G., Bosworth, H. B., Strauss, J. L., Stechuchak, K.M., Horner, R. D., et al. Lifetime sexual and physical victimization among male Veterans with combat-related post-traumatic stress disorder. Military Medicine. 2005, 170 (9): 787-790.
- Ogden, P, Minton, K, Pain, C. Trauma and the body: A sensorimotor approach to psychotherapy. New York: W. Norton & Co., 2006, pp. 41.
- Levine, P.A. In an unspoken voice: How the body releases trauma and restores goodness. Berkley CA: North Atlantic Books, 2010.
- Ogden, P, Minton, K, Pain, C. Trauma and the body: A sensorimotor approach to psychotherapy. New York: W. Norton & Co., 2006.
- Van der Kolk, B.A. The body keeps the score: Brain, mind, and body in the healing of trauma. New York: Penguin Books, 2015.
- Scaer, R. C., The body bears the burden: Trauma, dissociation, and disease. Second Edition. New York: Routledge, 2007.
- Ogden, P. Polyvagal theory and sensorimotor psychotherapy. In Porges, S.A. and Dana, D. (Eds), Clinical applications of the polyvagal theory: The emergence of polyvagal-informed therapies. New York: Guilford Press, 2018. pp. 34-49.
- Isaacson, W. Leonardo Da Vinci. New York: Simon and Schuster, 2017. Pp 212-13.
- Janet, P. Psychological healing: A historical and clinical study Vol. I. New York: The McMillan Co., 1925, p. 663.
- Ogden, P. and Fisher, J. Sensorimotor psychotherapy: Interventions for trauma and attachment. New York: W. Norton & Co., 2015 p. 776.
- Porges, S. W. The pocket guide to the polyvagal theory: The transformative power of feeling safe. New York: W. Norton & Co., 2017. Pp 19-20.
- Siegel, D. J. The developing mind: How relationships and the brain interact to shape who we are. New York: Guilford Publications, Inc., 2012 p. 281.
- Langmuir, J. L., Kirsh, S. G., Classen, C. C., A pilot study of body-oriented group psychotherapy: Adopting sensorimotor psychotherapy for group treatment of trauma. Psychological Trauma, Theory, Research Practice. 2012, 4 (2): 214-220.
- Ogden, P, Minton, K, Pain, C. Trauma and the body: A sensorimotor approach to psychotherapy. New York: W. Norton & Co., 2006, p. 27.
- Ogden, P. Polyvagal theory and sensorimotor psychotherapy. In Porges, S.A. and Dana, D. (Eds), Clinical applications of the polyvagal theory: The emergence of polyvagal-informed therapies. New York: Guilford Press, 2018. P. 46.
- Ogden, P, Minton, K, Pain, C. Trauma and the body: A sensorimotor approach to psychotherapy. New York: W. Norton & Co., 2006. p 187.
- Ogden, P, Minton, K, Pain, C. Trauma and the body: A sensorimotor approach to psychotherapy. New York: W. Norton & Co., 2006. pp 186-7.
- Ogden, P, Minton, K, Pain, C. Trauma and the body: A sensorimotor approach to psychotherapy. New York: W. Norton & Co., 2006. p. 187.
- sensorimotorpsychotherapy.org
ABOUT THE AUTHOR

Chris Zaglifa is a Licensed Clinical Social Work and Substance Abuse Counselor. He has worked as a child, adolescent, and family therapist in inpatient, outpatient, residential and hospital settings. His background includes work in a Victim Assistance Program, assistance in the development of a domestic violence shelter, and group work with children from violent homes. He later worked in the Crisis Intervention Services Program of the City of Chicago Department of Human Services. After moving to Wausau, WI, he worked as a clinical social worker at North Central Health Care Facilities on the inpatient unit, and on both the Behavioral Health unit and Emergency Department of Wausau Hospital. He was a member of the North Central Wisconsin Critical Incident Stress Management Team. He joined the staff at Family Counseling Services where mental health services were provided to families and to Veterans. Chris joined the Department of Veterans Affairs and worked full time with individuals and groups of Veterans for 11 years through November 2020. He completed Sensorimotor Psychotherapy Levels I, II, and III through the Sensorimotor Psychotherapy Institute.
Combat Stress Magazine
Combat Stress magazine is written with our military Service Members, Veterans, first responders, and their families in mind. We want all of our members and guests to find contentment in their lives by learning about stress management and finding what works best for each of them. Stress is unavoidable and comes in many shapes and sizes. It can even be considered a part of who we are. Being in a state of peaceful happiness may seem like a lofty goal but harnessing your stress in a positive way makes it obtainable. Serving in the military or being a police officer, firefighter or paramedic brings unique challenges and some extraordinarily bad days. The American Institute of Stress is dedicated to helping you, our Heroes and their families, cope with and heal your mind and body from the stress associated with your careers and sacrifices.

Leave A Comment
You must be logged in to post a comment.